Acne
Treating acne is one of the most difficult skin conditions that many of us will face during our lifetimes. We compiled a brief introduction to acne’s causes and some of the best ingredients available to treat pesky breakouts. Have more questions? Feel free to call or email us!
What Causes Acne?
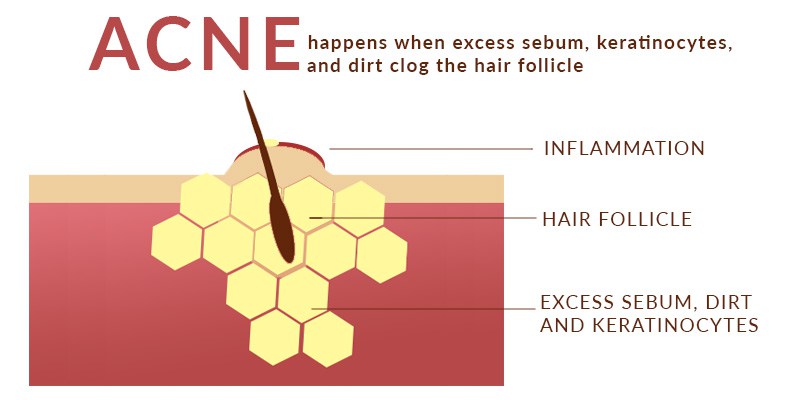
Unfortunately, we cannot offer you a satisfying answer about what precisely causes acne. Broadly, breakouts occur when excess sebum, keratinocytes, hair, or other debris clog the hair follicle. This in turn leads the pore to become swollen and eventually break. The spilled contents spread to the surrounding skin, which in turn causes acne. Although Propionibacterium acnes thrives on our skin naturally, it can become stuck with a clogged pore and exacerbate the inflammation (National Institute of Arthritis and Musculoskeletal and Skin Diseases, Mayo Clinic, American Academy of Dermatology). However, the triggers that lead to acne are not fully agreed upon.
There is compelling evidence that one’s diet may play a role in the development of acne. For example, several studies have suggested that dairy products and high glycemic indexes foods play a role in acne development. These findings are hotly contested among the research community, as there were several design flaws in each of the studies, and not all studies examined the same foods (i.e. some may have only examined different milks, whereas other included milk, cheese, ice cream, etc.) (DermatoEndocrinology, Acne.org, American Academy of Dermatology). Before ridding your diet of dairy and other beloved foods, consult with your dermatologist to see if this indeed is the source of your breakouts. We have included more links below if you wish to learn more about this topic.
Acne may also be induced by occupational factors. For example, if you work in a restaurant or a place where you frequently interact with greasy/oily substances, then these may collect on your skin’s surface (Mayo Clinic). If you also frequently rest your cheek on your hand, the oils from your hand may be transferring additional oil and germs to the face’s surface (Dr. Ava Shamban for HuffingtonPost.com). You should also be aware of cell phones, yoga mats, eyeglasses, and other surfaces which have extended contact with the skin and whose surfaces provide a hospitable habitat for bacterial colonization (Prevention.com, Everyday Health, Dr. Steven H. Dayan.) .
Acne may also be due to underlying medical conditions. For example, acne-rosacea and polycystic ovary syndrome both feature acne as prominent side effects (WomensHealth.gov, American Family Physician). Although the relationship is still under intense review, there is growing evidence that psychological stress may play a role in one’s acne development as well (Acta Dermato Venereologica, American Academy of Dermatology).
What Ingredients Should I Use for Acne-Prone Skin?
Salicylic acid
Of course we included salicylic acid on this list! This powerful exfoliating agent is great for breaking down the intercellular bonds between hardened skin cells so that your beautiful skin can shine through and flourish (Archives of Dermatological Research, British Journal of Dermatology). Evidence suggests that salicylic acid may also treat signs of post-inflammatory hyperpigmentation (such as scarring from acne), though more research is needed to support this claim (Dermatologic Surgery) Most importantly, research indicates that salicylic acid is more effective than benzoyl peroxide (the go-to ingredient in acne treatment) in treating acne breakouts and is generally far less irritating than benzoyl peroxide (Clinical Therapy). When used in low concentrations, salicylic acid may treat comedonal acne and psoriasis, whereas higher concentrations (10% – 40%) improved the appearance of warts and localized hyperkeratosis (Journal of the American Academy of Dermatology, Archives of Dermatological Research)
Lactic Acid
Lactic acid applied topically twice a day for one year was found to be a great at not only reducing the number of inflammatory and non-inflammatory acne lesions, but it also served as a great preventative ingredient against future outbreaks (Indian Journal of Dermatology, Venereology, and Leprology). Research published in the journal Archives of Dermatology suggested that lactic acid was also of benefit in improving signs of photodamage, such as rough skin, hyperpigmentation, and sallowness. Lactic acid (specifically its L-isomer) was also found to increase the number of ceramides (the waxy molecules that comprise the skin barrier) in skin. This in turn resulted in a fortified skin barrier that limited transepidermal water loss and improved the appearance of xerotic skin (Archives of Dermatological Research)
Azealic Acid
Chances are that you have never heard of azelaic acid before, but don’t be so quick to dismiss it. Azelaic is believed to prevent/treat melanin formation by both damaging melanocytes and impeding melanocyte proliferation cells (Drugs), which may be of benefit in treating acne-induced hyperpigmentation. However, a similar study suggested that azelaic acid combined with tretinoin provides more efficacious treatment for hyperpigmentation (Cutis) Even better, research published in Acta Dermato Venereologica Supplementum,(Stokholm) found that topically-applied azelaic acid is just as effective as treinoin (retinoic acid) when it comes to treating acne but is generally less irritating to the skin. When paired with glycolic acid, azelaic acid was found to treat mild to moderate acne lesions (Clinical Therapy). Additionally, recent research suggests that azelaic acid can be of benefit in treating moderate papulopustular rosacea, a condition characterized by inflammed red skin, flushing, and pimple outbreaks (Journal of the American Academy of Dermatology)
Retinoic Acid
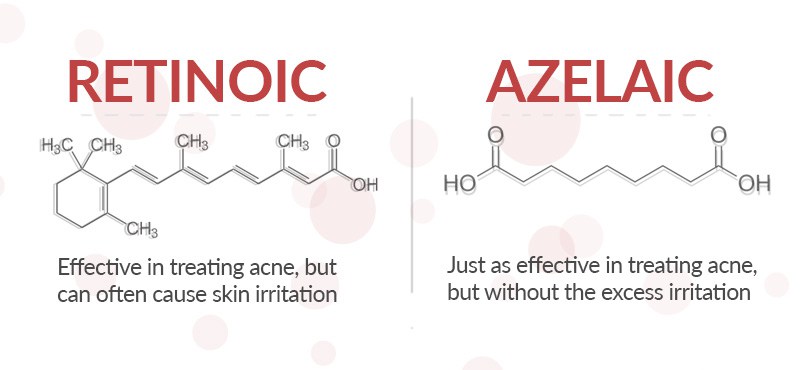
Retinoic acid (tretinoin) has long been used to fight acne. According to research published in the New England Journal of Medicine, topically-applied retinoic acid can significantly improve discoloration in hyperpigmented acne lesions. However, despite its efficacy in treating inflammatory and non-inflammatory acne lesions, topical retinoic acid may induce temporary inflammation or discomfort, so those with sensitive skin should consult with a dermatologist before using it (International Journal of Dermatology). Studies have repeatedly found that topically-applied retinoic acid can also improve the appearance of photo-damaged skin, a bonus for those of us who need to treat multiple conditions concurrently (JAMA Dermatology, Journal of Dermatological Treatment)
Glycolic Acid
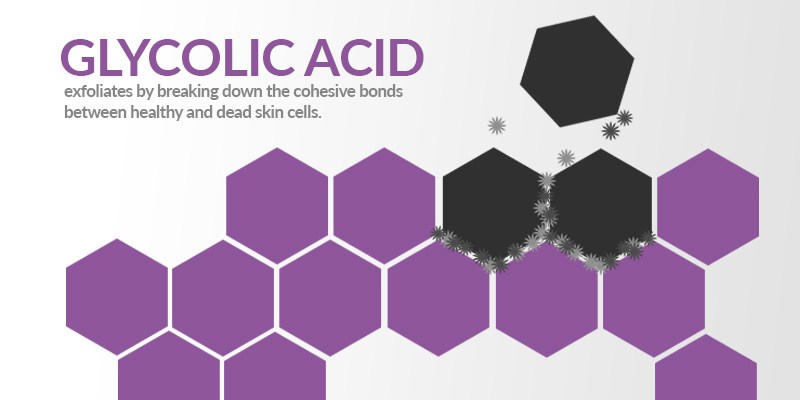
Although not quite as strong as retinoic acid when it comes to exfoliation, glycolic acid is still a force to be reckoned with. Not only does glycolic acid exfoliate the skin by breaking down the cohesive bonds between cells, but it also soothes erythematous skin and offers a small degree of photoprotection (BioMed Research International, Dermatologic Surgery). According to research published in the Egyptian Journal of Histology, glycolic acid can also treat hyperpigmentation by altering melanocytes. The same study also found that glycolic acid increased the number of active fibroblasts and bundles of dense collagen in guinea pig skin, meaning that glycolic acid not only exfoliates skin, but it can soothe inflamed lesions and return skin to a more healthy form.
Gluconolactone
Despite its funny name, gluconolactone doesn’t mess around. Research from the Australian Journal of Dermatology found that gluconolactone was just as effective as benzoyl peroxide in treating inflamed and non-inflamed acne lesions, but generally was less irritating then benzoyl peroxide. As an added bonus, gluconolactone also is a great free radical scavenger and is also known to provide a strong defense against transepidermal water loss (Allergy and Therapy)
Which ViaBuff Should I Use?

If you suffer from acne (especially if you have oily or sensitive skin and acne), then we suggest using the ViaBuff Level 1 Exfoliating Puff, which was designed for suffers of psoriasis, oily skin, sensitive and acne-prone skin in mind. This puff was designed from an open-cell polyurethane that discourages bacterial colonization by limiting water retention. So what does that mean for your skin? Because the design promotes rapid air drying, you don’t have to worry about bacteria growing on your puff and further infecting your skin whenever you exfoliate. Our puffs were also designed to be gentle enough to exfoliate inflamed or sensitive lesions without inducing further pain. Even better, our puffs last for an average of 90 days, or more than three times longer than your standard puffs and loofahs. However, many of our clients report using them for several months before having to be replaced!



